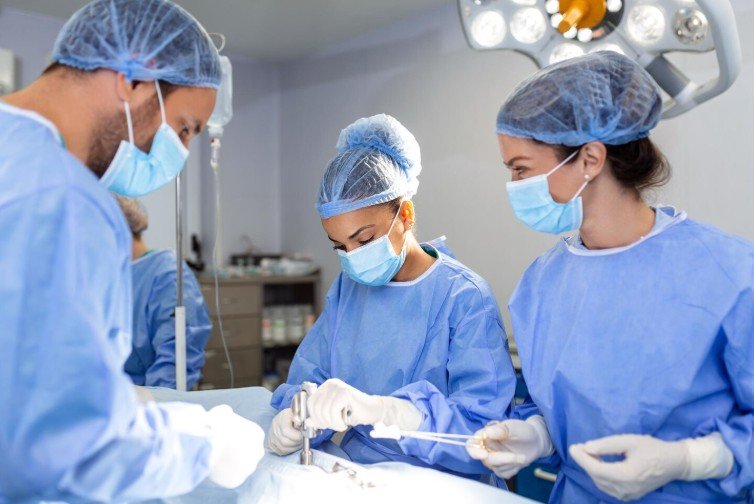
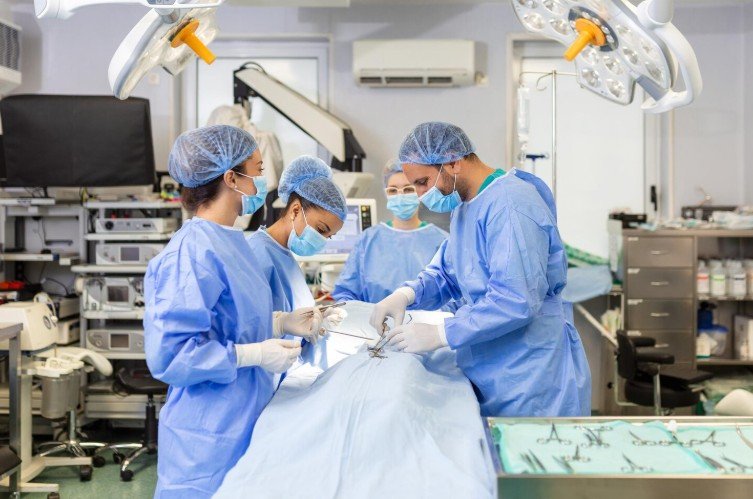
Over the past few decades, gynecologic surgery has undergone a remarkable transformation. Traditional open surgeries that required large incisions, longer hospital stays, and extended recovery periods are now increasingly being replaced by minimally invasive surgical techniques. These modern procedures allow surgeons to treat complex gynecological conditions with smaller incisions, greater precision, and faster patient recovery.
Minimally invasive gynecologic surgery includes techniques such as laparoscopy and robotic-assisted surgery, which have become the preferred approach for many procedures including hysterectomy, fibroid removal, ovarian cyst surgery, and treatment of endometriosis.
According to experts like Dr. Shweta Mendiratta, recognized as one of the best gynecologists in Faridabad, continuous innovations in surgical technology are further improving outcomes for women. From advanced robotic systems to artificial intelligence-assisted planning, the future of gynecologic surgery is evolving rapidly.
In this article, we explore the latest advances in minimally invasive gynecologic surgery, emerging technologies shaping the future, and how these developments benefit patients.
Understanding Minimally Invasive Gynecologic Surgery
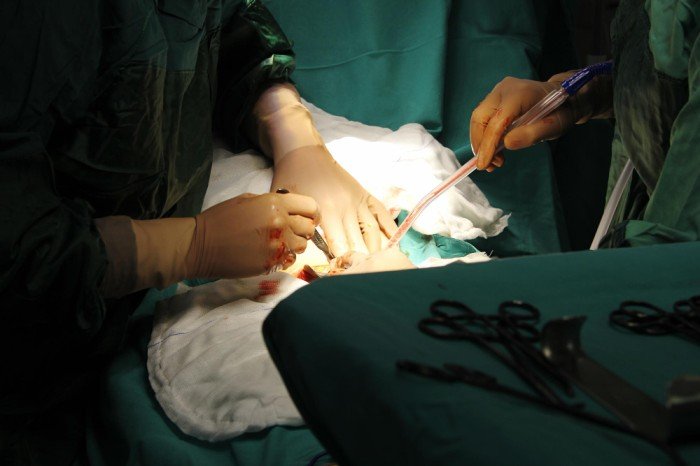
Minimally invasive surgery (MIS) refers to surgical techniques that are performed through small incisions using specialized instruments and cameras rather than large cuts used in traditional open surgery.
Common minimally invasive approaches include:
- Laparoscopic surgery
- Robotic-assisted surgery
- Hysteroscopic procedures
These techniques allow surgeons to operate with enhanced precision while minimizing trauma to surrounding tissues.
Why Minimally Invasive Surgery Is Transforming Women’s Healthcare
Minimally invasive surgery has become increasingly popular because it offers several advantages for patients:
- Smaller incisions
- Less post-operative pain
- Reduced blood loss
- Shorter hospital stays
- Faster recovery
- Minimal scarring
These benefits not only improve surgical outcomes but also enhance the overall patient experience.
Emerging Trends in Minimally Invasive Gynecologic Surgery
As technology continues to evolve, several new innovations are shaping the future of gynecologic surgery. These advancements are designed to improve surgical precision, reduce complications, and further enhance patient safety.
- Single-Incision Laparoscopic Surgery (SILS)
One of the latest innovations in minimally invasive surgery is Single-Incision Laparoscopic Surgery (SILS).
Unlike conventional laparoscopy, which requires multiple small incisions, SILS involves performing the entire surgery through a single small incision, usually near the belly button.
Advantages of SILS
- Minimal visible scarring
- Reduced post-operative pain
- Faster healing
- Improved cosmetic outcomes
Although SILS requires specialized training and equipment, it is becoming increasingly popular for procedures such as hysterectomy and ovarian cyst removal.
- Augmented Reality in Surgical Planning
Another exciting advancement in surgical technology is the use of augmented reality (AR) in surgical planning.
Augmented reality allows surgeons to combine 3D imaging from CT scans or MRIs with real-time surgical views, providing a more detailed understanding of the patient’s anatomy.
Benefits of Augmented Reality
- Better surgical planning
- Improved visualization of organs and blood vessels
- Greater surgical accuracy
- Reduced risk of complications
AR technology helps surgeons navigate complex cases with greater confidence and precision.
- AI-Assisted Robotic Surgery
Artificial Intelligence (AI) is beginning to play an important role in surgical innovation. In robotic-assisted procedures, AI-powered systems can assist surgeons by analyzing data and providing insights during surgery.
How AI Supports Robotic Surgery
- Predicting potential complications
- Assisting in surgical decision-making
- Enhancing robotic instrument precision
- Providing real-time feedback
Although AI does not replace surgeons, it serves as an intelligent support system that helps improve surgical outcomes.
- Improved Suturing Tools and Energy Devices
Technological advancements are also improving the tools surgeons use during procedures.
Modern energy devices and suturing instruments allow surgeons to perform delicate tasks more efficiently.
Examples of Advanced Surgical Tools
- Advanced bipolar energy devices for precise tissue sealing
- Ultrasonic surgical instruments
- Improved laparoscopic suturing devices
- Advanced robotic instruments with enhanced flexibility
These innovations help reduce surgical time, minimize bleeding, and improve patient recovery.
How These Advances Benefit Patients
Technological innovations in gynecologic surgery are not just about improving surgical techniques — they are also about improving the overall patient experience.
Faster Recovery
Modern minimally invasive procedures cause less tissue damage, allowing patients to recover faster and return to daily activities sooner.
Reduced Surgical Complications
Advanced imaging and robotic systems help surgeons operate with greater accuracy, reducing the likelihood of complications.
Greater Precision
Robotic and AI-assisted technologies enable surgeons to perform extremely delicate procedures with enhanced control.
Improved Patient Comfort
Smaller incisions and less trauma to surrounding tissues lead to reduced pain and minimal scarring.
These benefits are transforming the way gynecological conditions are treated.
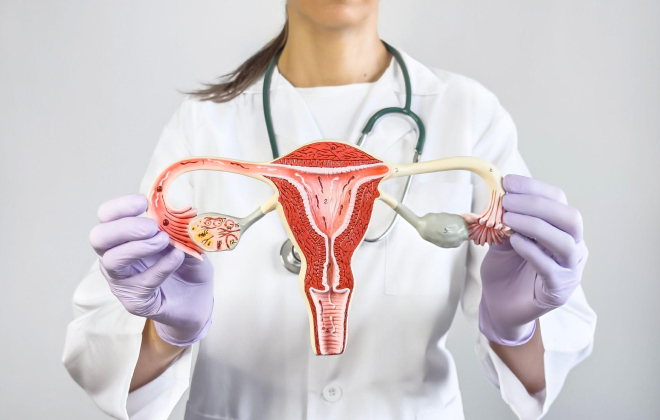
Conditions Treated Using Advanced Minimally Invasive Surgery
Minimally invasive techniques can be used to treat a wide range of gynecologic conditions, including:
- Uterine fibroids
- Endometriosis
- Ovarian cysts
- Adenomyosis
- Pelvic organ prolapse
- Chronic pelvic pain
- Infertility-related conditions
- Gynecologic cancers (early stage)
Many of these procedures can now be performed with robotic or laparoscopic techniques, allowing for better surgical outcomes.
The Importance of Surgical Expertise
While modern technology plays a crucial role in advancing surgical care, the expertise of the surgeon remains the most important factor in achieving successful outcomes.
Experienced specialists such as Dr. Shweta Mendiratta, widely regarded as one of the best gynecologists in Faridabad, combine advanced surgical technology with years of clinical expertise to provide safe, effective, and personalized treatment for women.
Choosing an experienced surgeon ensures that patients benefit fully from the latest advancements in minimally invasive gynecologic surgery.
The Future of Gynecologic Surgery
The field of gynecologic surgery continues to evolve rapidly, and several exciting innovations are expected in the coming years.
Future developments may include:
- Fully integrated AI-assisted robotic platforms
- Enhanced surgical simulation and training tools
- Personalized surgical planning using genetic and imaging data
- Advanced micro-robotic surgical instruments
These technologies aim to make surgeries even safer, more precise, and more patient-friendly.
Conclusion
Minimally invasive gynecologic surgery has revolutionized women’s healthcare by providing safer alternatives to traditional open surgery. With smaller incisions, faster recovery, and reduced complications, these techniques have become the preferred approach for treating many gynecological conditions.
The future of gynecologic surgery is even more promising. Emerging technologies such as single-incision laparoscopic surgery, augmented reality, AI-assisted robotic systems, and advanced surgical instruments are shaping the next generation of surgical care.
As innovation continues to advance, patients can expect smarter, safer, and more personalized treatment options.
With the guidance of experienced specialists like Dr. Shweta Mendiratta, women can benefit from these modern surgical techniques and achieve better health outcomes with minimal disruption to their daily lives.
FAQs
- What is minimally invasive gynecologic surgery?
Minimally invasive surgery involves performing procedures through small incisions using specialized instruments and cameras. It reduces pain, scarring, and recovery time compared to traditional open surgery.
- Is robotic surgery safer than traditional surgery?
Robotic surgery offers improved precision, better visualization, and smaller incisions, which often result in fewer complications and faster recovery when performed by an experienced surgeon.
- How long does recovery take after minimally invasive surgery?
Most patients recover within 1–3 weeks, depending on the procedure and their overall health condition.
- Are these surgeries painful?
Because minimally invasive surgeries use small incisions, patients generally experience less pain compared to open surgery. Pain can usually be managed with medication.
- Who is a good candidate for minimally invasive gynecologic surgery?
Many women with conditions such as fibroids, ovarian cysts, endometriosis, or pelvic pain may be candidates. A consultation with a specialist will determine the most appropriate treatment.